Neurofeedback: How to Retrain Your Brain
Addiction and co-occurring disorders change the way the brain functions. One of the ideal goals for recovery is to restore the brain back to a healthy state of functioning, but it’s historically been difficult to get an objective picture of the brain in action. Instead, we have always relied on behavioral and psychological measures. However, new and cost-effective technologies now give us the opportunity to monitor brain activity in real-time.
During treatment we want to offer our patients every possible tool to help them address their substance use and co-occurring disorders. There are several approaches to treatment, including cognitive-behavioral therapies and psychological counseling, as well as pharmacological approaches that manage symptoms. Neurofeedback fits within the non-pharmacological modalities, providing an additional clinical tool beyond the paradigm of “give me a pill to fix my pill problem,” while highlighting the importance of comprehensive approaches to treatment.
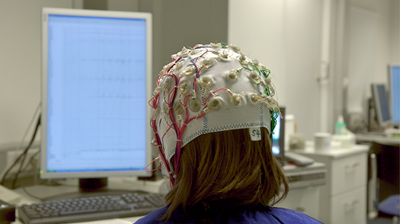
One of the technologies in use at Caron is Electroencephalography, or EEG, which detects very small changes of electrical activity in the brain. A net of EEG sensors, that looks like a shower cap, is put over the patient’s head, and some gel is used to improve electrical connectivity. As the patient completes various tasks, the brain generates electrical activity, which is detected by the EEG sensors and then sent to a computer. The computer analyzes these signals and provides the patient a simplified picture of what their brain is doing. This process creates a feedback loop that helps patients understand the relationship between their brain activity and what they think and feel.
It’s as if we’re holding up a mirror to the patient, but this mirror reflects the brain activity they’re experiencing in that moment. For the first time, they’re getting a reflection of what’s happening underneath the surface of their own internal experience, the underlying brain function that relates to why they feel the way they feel and how they think the way they think.
The ”feedback” part of neurofeedback is usually something visual and is often presented to the patient in the form of a game, perhaps a race car driving around a racetrack. The goal of the game is simply to get the car to move forward. There’s no need to worry about steering; you just have to get the car to move. The incredible thing about this game is that there’s no remote control. The car’s movement is, instead, tied to brain activity. In other words, you don’t drive this car with your hands; you drive it with your mind. What makes the car move will be different for different people, depending on the specific brain function we need to address during treatment. But the key is that, as the patient gets better at driving the car, what they’re really doing is learning how to better-regulate their brain function. In the same way that people go to the gym to build strength in their bodies, patients at Caron can use neurofeedback sessions to improve the activity of their brains.
In addition to neurofeedback, there has been a great deal of research simply to characterize longitudinal changes in the brain during active addiction and in recovery. How long into recovery does the brain still appear as though it’s been affected by addiction? Is it two weeks, two months, two years? We’re still learning the answers to these questions, as well as how neurofeedback could be used to help accelerate the process.
Many studies have focused instead on using neurofeedback to address co-occurring disorders like anxiety or attention deficit. Most of our patients also have mental health disorders such as these, and neurofeedback can be a great help here. If these underlying mental health disorders aren’t addressed, then they themselves pose a threat for someone relapsing. Someone with generalized anxiety will likely continue to experience moments where they simply want relief from their anxiety, putting them at risk for returning to the alcohol, benzodiazepine, or opioid habits they once used to cope.
Importantly, neurofeedback requires that people take an active role in working through their own feelings and their own well-being. It is first and foremost an exercise in self-regulation. One of the simple truths of recovery is that someone must be actively engaged in the process or else they won’t progress. The same is true for neurofeedback.
We’ve learned a tremendous amount about how the brain functions in addiction over the past 20 to 30 years. At the same time, that knowledge really hasn’t been applied clinically to help change people’s lives. Part of the problem is that many of the technologies to monitor brain function, such as functional magnetic resonance imaging (fMRI), are too expensive and complex to be used outside of large hospitals or research centers. Newer technologies, smaller and less expensive, are now making it possible to monitor brain activities in an everyday setting. Neurofeedback is an innovative, evolving modality that adds to our clinical toolbox and helps improve the way we treat addiction and co-occurring disorders. It’s very exciting, and we’re looking forward to seeing how things continue to grow and develop over the next several years.
Related Content
Take the next step:
- Caron in Pennsylvania 1-800-854-6023
- Caron in Florida 1-800-221-6500
- Breakthrough at Caron 1-800-213-7834
Start with an online form



