Insurance Options
Increasing access to high-quality treatment
Insurance Agreements Offer Access to Caron’s Care
Caron Treatment Centers is in-network with several insurance providers, enabling more people to get high quality treatment for substance use disorder in-network, making it available at a lower cost to patients.
Caron is in-network with several providers:
Creating these agreements ensures that Caron makes life-saving addiction treatment available to more individuals and families, guiding them on a four-week, transformational journey that will serve as the first steps in achieving Recovery for Life. These agreements negotiated by Caron provide for a minimum 28-day stay at the Caron Pennsylvania campus only. Some program exclusions may apply based on insurance provisions, such as, but not limited to Capital Blue Cross and FEP. Your costs for treatment will be subject to your deductible, co-insurance, and/or co-pays.
- Aetna
- Highmark BlueCross BlueShield: This agreement allows those seeking treatment to access programming through the Blue Cross Blue Shield (BCBS) Association’s Blue Card Program.
- AmeriHealth New Jersey (AmeriHealth/Independence Administrator)
- Independence Blue Cross (Keystone Health Plan East/Personal Choice)
- Quest Behavioral Health (Tower Health/Penn Medicine)
- UPMC (Pinnacle Health)
Caron’s core programs provide:
- Inpatient treatment based on a minimum 28-day length of stay, relieving patients and families of the burden of paying for care that extends beyond detox and offering a foundation for sustained recovery.
- Patient-to-staff ratios that are among the lowest in the industry
- An individualized treatment plan with components specifically tailored to meet the level of care needed and treat substance use disorder as well as other physical or behavioral health conditions
- A team of addiction medicine experts to manage the course of treatment independently of managed care concurrent reviews
- Treatment of substance use disorder as a chronic disease through the implementation of a disease-management plan. (That plan may require additional treatment that may not be covered by your insurance provider.)
Advancing Value-Based Care for Better Rates of Recovery
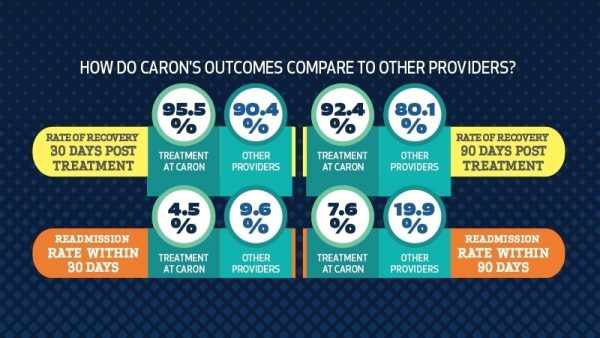
Our value-based care model for substance use disorder improves patient access, coordination, experience of care, and the overall quality of life for those seeking treatment. Based upon recent independent studies from two leading insurance providers that evaluated 90-day readmission rates, a treatment model that prioritizes a medically-appropriate, interdisciplinary, patient-centric treatment plan – like the one we use at Caron – can significantly improve patient outcomes and rates of recovery.
Our Treatment Model Works
Contact Us
Take the next step:
Start a conversation
Start with an online form
-
Caron in Pennsylvania
1-800-854-6023 -
Caron in Florida
1-800-221-6500 -
Breakthrough at Caron
1-800-213-7834

